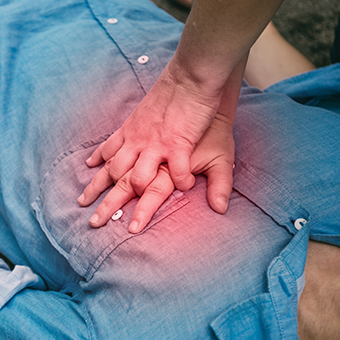
Providing courageous help despite the risk of infection - adapted guidelines for cardiac massage
Since the global corona pandemic 2020, we know how important infection protection is. Wearing masks, washing hands regularly and keeping a distance of at least 1.5 metres make up the core of these protective measures. But what to do if someone collapses and needs help? A scenario that was already highly fearful before the pandemic. Now there is the added uncertainty of a possible infection with SARS-CoV-2. It is therefore all the more important to familiarize oneself with the adapted recommendations for first aid and cardiac massage.
In Germany, between 60 and 70 thousand people die every year from cardiovascular arrest. In most cases, there is first a loss of blood circulation, then respiratory arrest and clinical death. Prompt resuscitation is possible in principle. However, neither pure cardiac massage nor cardiac massage in combination with mouth-to-mouth or mouth-to-nose resuscitation is aimed at such resuscitation. Rather, the aim is to prevent the irreversible death of important organs by maintaining the cardiovascular function. Lay "resuscitation" therefore serves to bridge the gap until the heart can be resuscitated with the help of a defibrillator or the administration of appropriate medication. However, without the prior assistance of laypersons, successful resuscitation becomes unlikely. Even if resuscitation is successful, if cardiac massage is performed too late or too hesitantly, the brain may not be supplied with oxygen-rich blood. This can result in permanent brain damage. So it is important to provide help.
In adults, heart problems usually lead to circulatory arrest. If the heartbeat stops completely, circulatory arrest is inevitable. But an infarction or cardiac arrhythmia can also lead to circulatory arrest. Strokes or lung diseases are less frequent causes. It is currently not possible to determine how often cardiovascular arrest occurs in connection with Covid-19.
In a cardiac arrest caused by heart problems, the person quickly loses consciousness. After about half a minute, there is a gasping respiration, i.e. abrupt, short and irregular breathing that does not provide a regular air supply to the body. Afterwards, breathing stops completely. This process is also called sudden cardiac death. However, actual death can still be averted through cardiac massage and subsequent resuscitation.
Often, such an emergency does not occur in public, but in households. However, the procedure for first responders is the same in both cases. If a person collapses or is found lying down and apparently unconscious, the first thing to do is to check whether the person is still responsive. Shaking the shoulders is not recommended because of the risk of infection. If there is no response to loud shaking, check for breathing. Before the Covid 19 pandemic, it was recommended to approach the face of the person in need of help.
According to the new guidelines, it is sufficient to check breathing visually. The gasping breathing described above does not count as regular breathing. If the chest or abdomen does not visibly rise and fall, not only must an emergency doctor be called, but CPR must also be started. A second person can help while maintaining a safe distance, and stay in contact with the emergency services. The telephone call must not be terminated without prompting. The staff can provide assistance with CPR until the ambulance arrives and may still need to ask questions, for example if the location is not clear. If no other person is present, the hands-free function of the telephone can also be activated for this purpose. Even before the pandemic, the administration of combined cardiopulmonary resuscitation by laypersons was not advocated by all sides. Even before Covid-19, the German Heart Foundation recommended that only cardiac massage be performed until either the emergency doctor or an Automated External Defibrillator (AED, also called a lay defibrillator or defi for short) arrives. The administration of cardiac massage without ventilation can be successful because in the case of collapse due to cardiac arrest, the saturation of the blood with oxygen is still sufficient for a few minutes. Mechanical action on the heart muscle from the outside can then replace normal heart function and keep the blood flow going. For this to succeed and for blood to travel throughout the body and especially to the brain, sufficient force must be applied. This means that the sternum must be pushed in about 5 to 6 cm deep at about the level of the nipples. To ensure this, the elbows of the person providing assistance should be pushed through. If the incident occurred at home, the collapsed person may be lying on a soft surface that prevents effective cardiac massage, for example a sofa or mattress. In this case, the person should be placed on a hard surface. Especially if the person is wearing thick winter clothing, it may be useful to open it for cardiac massage. This way, the pressure is not cushioned and the correct hand position can be better assessed. However, the German Heart Foundation is against removing the clothing, as this can cost important seconds. The frequency with which the massage has to be done is quite high and is 100 to 120 strokes per minute, which roughly corresponds to the beat of the Bee Gees classic "Stayin' Alive". As this is very strenuous in the long run, it makes sense to take turns with a second person if possible. An innovation in the course of the pandemic is the recommendation to put a light, thin piece of cloth or a paper handkerchief over the mouth and nose of the person in need of help, unless he or she is already wearing a mouth-nose covering. Although the person in this scenario is not breathing, it is still likely that aerosols will be emitted by the pressure massage. The helper can also wear a mask or quickly put one on. Only when the emergency doctors who have arrived or the automatic announcement of the AED ask to do so, may the massage be stopped. A lay defibrillator can now be found at many points in public spaces, for example in train stations, hotels and offices. If more than one person is providing assistance, a defibrillator may be fetched while chest compressions continue. When the defibrillator arrives, the instructions for applying electrodes must be followed. The device then analyses the physical situation of the person in need of help, guides those providing assistance and decides whether an electric shock is necessary or not.
In the wake of the Covid 19 pandemic, the German Heart Foundation has issued an urgent warning that the willingness to provide assistance could decline, resulting in an increase in preventable deaths. To help you deal with your fear of possible infection and of doing something wrong in an emergency, we have summarized the adapted guidelines once again:
Easy to remember: Check - Call - Press - Shock
Check: Check the collapsed person for unconsciousness and breathing. Does the person respond to being approached and called? Does the chest or abdomen rise and fall regularly?
Call: Dial the emergency number. The emergency number is 112 throughout the EU. Do not hang up hastily, but wait to be asked.
Press: If the person is unconscious and not breathing or is gasping for breath, start chest compressions. Cover the person's mouth and nose with a thin cloth. Place both hands on top of each other on the centre of the person's chest. Extend your elbows and press down firmly and vertically 100 to 120 times per minute. The chest should lower noticeably, about 5 to 6 cm deep. The frequency corresponds to the beat of "Stayin' Alive". Do not stop until instructed to do so by the rescue team or the defibrillator instructions.
Shock: If another person brings a lay defibrillator to the emergency scene, you can use it to continue treating the collapsed person. The defibrillator will give instructions on how to do this.
Information material on resuscitation and other cardiac topics is also available on the website of the German Heart Foundation



