Diabetes mellitus
Diabetes mellitus - Die wichtigsten Fakten
Welche Typen von Diabetes gibt es?
Welche Folgeerkrankungen können durch Diabetes entstehen?
Diabetes mellitus - Die wichtigsten Fakten
Diabetes mellitus (Zuckerkrankheit) kennzeichnet eine chronische Stoffwechselerkrankung, die zu einem erhöhten Blutzuckerspiegel (Hyperglykämie) führt. Dabei ist das Risiko für schwere Begleit- und Folgeerkrankungen sehr hoch.
Um den Körper mit ausreichend Energie zu versorgen benötigt dieser Glukose. Eine bestimmte Menge an Glukose befindet sich immer im Blut, um diese jederzeit, z. B. für plötzliche Belastungen, bereitstellen zu können. Der sogenannte Blutzuckerspiegel liegt bei gesunden Menschen zwischen 80 bis 120 Milligramm pro Deziliter (mg/dl).
Nach der Aufnahme von Nahrung schüttet die Bauchspeicheldrüse (Pankreas) das Hormon Insulin aus, damit die Zellen die benötige Glukose aufnehmen können. Das Insulin wird in den sogenannten Langerhansschen Inseln produziert. Diese liegen millionenfach in Form von Inseln in der Bauchspeicheldrüse verteilt. Insulin bindet sich an die Oberfläche der Zellen, diese werden aktiviert und können nun Glukose aufnehmen. Besteht ein Mangel an Insulin, bleibt der Zucker im Blut zurück, der Blutzuckerspiegel steigt und der Körper greift auf das Fettgewebe als Energiequelle zurück.
Welche Typen von Diabetes gibt es?
Es werden neben seltenen Diabetes-Sonderformen, wie z.B. Schwangerschaftsdiabetes, zwei Typen unterschieden: Typ 1 Diabetes und Typ 2 Diabetes. Dabei tritt Typ 1 wesentlich seltener auf als Typ 2, der in etwa bei 95 Prozent der Betroffenen vorliegt. Umgangssprachlich wird Diabetes mellitus auch als Zuckerkrankheit bezeichnet. Dieser Begriff hat seinen Ursprung darin, dass Diabetiker mit ihrem Urin Zucker ausscheiden.
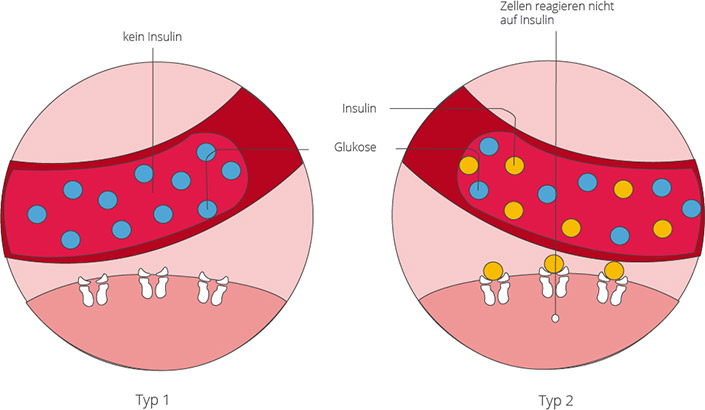
Diabetes Typ 1
Diese Diabeteserkrankung beginnt oft in der Kindheit oder Jugend, meist zwischen 11 und 13 Jahren und beruht auf einem Mangel des Hormons Insulin. Infolge einer Zerstörung der insulinproduzierenden Zellen (Beta-Zellen) in der Bauchspeicheldrüse, durch bestimmte weiße Blutkörperchen (T-Lymphozyten), reduzieren sich die insulinproduzierenden Zellen drastisch und nicht genug Glukose kann in die Zellen gelangen. Dieser Prozess ist die Folge von erblichen Veranlagungen, äußeren Faktoren (z.B. bestimmte Virusinfektionen wie Mumps- und Rötelnviren) und einer Fehlsteuerung des Immunsystems.
Symptome Typ 1:
Die Symptome bei Diabetes Typ 1 treten erst auf, wenn schon 80 Prozent der insulinbildenden Zellen verschwunden sind. Dazu zählen:
- Starker Durst
- Vermehrtes Wasserlassen
- Heißhunger
- Juckreiz
- Abgeschlagenheit
- Anfälligkeit für Infekte
Zwischen dem Beginn der Erkrankung und dem Auftreten der ersten Symptome können Wochen, Monate oder sogar Jahre liegen.
Betroffene mit Diabetes Typ 1 müssen regelmäßig Insulin spritzen um den Mangel des Hormons auszugleichen. Das Fortschreiten der Krankheit lässt sich zu Beginn nur kurzfristig verlangsamen, schreitet aber fort bis alle insulinproduzierenden Inselzellen zerstört sind und der Körper kein eigenes Insulin mehr produzieren kann.
Diabetes Typ 2
Der Diabetes Typ 2 tritt meist bei älteren Menschen auf und wird deshalb auch oft als „Altersdiabetes“ bezeichnet. In den letzten Jahren hat sich das Alter beim ersten Auftreten des Diabetes zunehmend nach unten verlagert und vermehrt jüngere Menschen bis hin zu Kindern weisen diesen Typ auf.
Faktoren für diesen Typ sind Körperzellen, die zunehmend unempfindlicher auf das Insulin reagieren und obwohl sie es benötigen dieses nicht mehr aufnehmen. Die Körperzellen werden gegenüber dem aus der Bauchspeicheldrüse ausgeschütteten Insulin resistent und der Blutzuckerspiegel steigt. Um diesen dennoch niedrig zu halten produziert die Bauchspeicheldrüse immer mehr Insulin nach. Nach jahrelanger, starker Belastung der Inselzellen lässt die Produktion nach und es wird immer weniger Insulin produziert. Faktoren welche die Insulinresistenz bedingen sind fettreiche Kost, starkes Übergewicht vor allem am Bauch, Bluthochdruck und Bewegungsmangel. Genetisch Vorbelastete müssen besonders auf einen gesunden Lebensstil achten.
Symptome Typ 2:Lange Zeit treten keine Symptome auf, erst mit dem Auftreten von Folgeerkrankungen wird die Krankheit bemerkt.
Welche Folgeerkrankungen können durch Diabetes entstehen?
Wird der Blutzuckerspiegel auf Dauer nicht reguliert hat dies zur Folge, dass die Blutgefäße nachhaltig geschädigt werden und Folgeerkrankungen auftreten. Zu den Folgeerkrankungen zählen:
- Veränderungen der Netzhaut (diabetische Retinopathie)
- Störungen der Nierenfunktion (diabetische Nephropathie)
- Herzinfarkt
- Schlaganfall
- Erektionsstörungen
- Anfällig für Infekte und
- Durchblutungsstörungen der Beine und Füße.
Treten Taubheitsgefühle und Gefühlsstörungen auf, können Nerven nachhaltig durch Diabetes mellitus geschädigt sein. Hier muss eine lebenslange und sorgfältige Blutzuckereinstellung vorgenommen werden.
Die häufigste auftretende Komplikation bei Diabetes mellitus ist der diabetische Fuß. Nervenschäden und Durchblutungsstörungen in den Füßen führen zu offenen, schlecht heilenden Wunden und Geschwüren.
Allerdings können Diabetes Typ 2-Betroffene zu Beginn der Erkrankung mit einer Änderung des Lebensstils einiges abwenden. Viel Bewegung, ein normales Gewicht und eine gesunde Ernährung können bereits den Blutzuckerspiegel stabilisieren. Ist die Erkrankung schon weiter fortgeschritten, müssen Medikamente oder Insulinspritzen verschrieben werden um den Blutzucker zu regulieren.
